Dental subluxation is a traumatic injury to the periodontal tissue in which the tooth has increased mobility (i.e., is loosened) but has not been displaced from its tooth socket.
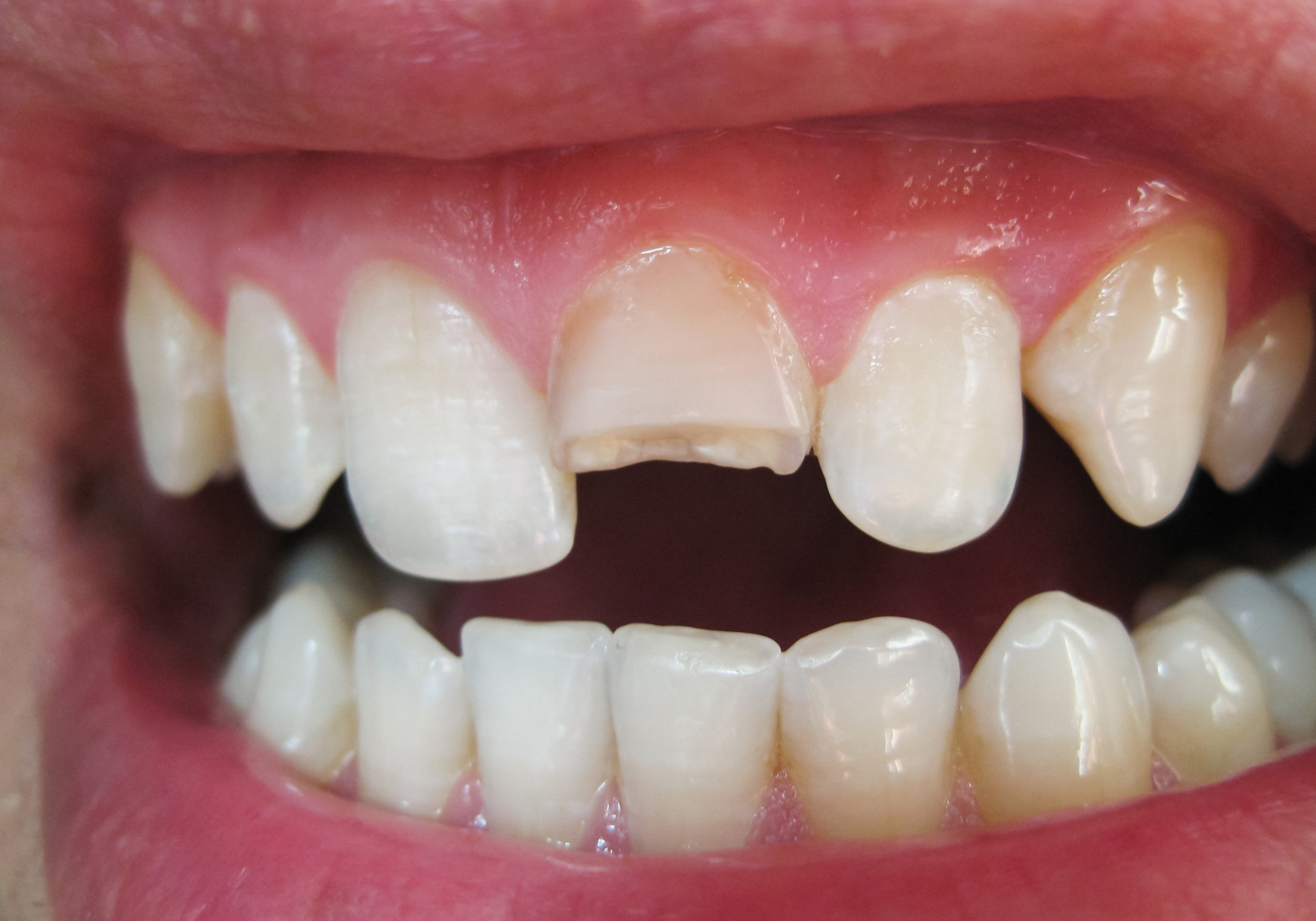
High impact force during trauma causes damage to the periodontium and results swelling and bleeding from the gingival sulcus. Trauma also causes rupture of some periodontal fibres and this leads to loosening of the tooth. However, the force is not strong enough to cause displacement of the tooth from its socket. Sometimes, the trauma might cause pulpal damage and there is a minimal risk of pulpal necrosis, thus follow-up is essential
A tooth that has been subluxated shows symptoms of being tender to percussion (tapped using the end of the mirror) and tender to palpate around the area and/or sulcus as it has been slightly mobilised yet remains undisplaced. To begin with, any sensitivity testing of the pulp may provide a negative response; in which case it is important to continue monitoring until a pulpal response is received.
Radiographically, there are no unusual features to note in a subluxated tooth. However, it is important to focus on the full image and scan for any other areas which may have also been affected; something which the patient may not actually have noticed or complained of. If there is any suspicion of a root fracture, it is recommended to take an occlusal exposure radiograph to allow for a definitive diagnosis. Taking radiographs is useful as they can be referred to in case of any future complications.
When a patient presents to the dentist following any form of dental trauma, a full and thorough clinical assessment should be carried to exclude more serious injuries that may require urgent management.
The first stage of the clinical assessment is to take a complete history to rule our head injury or inhalation of particles. Questions to obtain this information include:
· Did the patient lose consciousness?
· Were there any witnesses?
· Has the patient had any nausea or vomiting since the incident?
· Is there any loss of memory?
· Can all particles be accounted for
· Is the patient experiencing any change in vision?
If there is any doubt of head injury or aspiration, the patient should attend the nearest accident and emergency service prior to receiving dental treatment.[7]
Having ruled out serious injuries, it is then important to undertake a full trauma, dental and medical history. This will include understanding if the patient is currently having symptoms, has a history of dental trauma, and their tetanus status.
Following a complete history, a clinical examination is then undertaken.
Extra-oral examination includes:
· Cleaning cuts with saline solution and removal of foreign bodies
· Palpation of the entire facial skeleton to rule out fractures
· Assessment for abnormalities in mandibular opening
· Checking for bruising
Intra-oral examination includes checking for:
· Bruising
· Blood clots
· Cuts/ lacerations
· Tooth mobility
· Fractured teeth
· Changes to occlusion
Following subluxation of a primary tooth there is no active treatment required. The patient should be advised to keep the area as clean as possible by swabbing with 0.12% chlorohexidine twice daily. Clinical follow up will be carried out at 1 week and 6–8 weeks after injury. Follow up radiographs are not required unless complications occur.
Management is similar to primary teeth. No active treatment is usually required however a flexible splint may be placed for up to 2 weeks if the patient is experiencing extreme discomfort. Follow up to check for complications is more frequent. Radiographical and clinical exam should be carried out at 2 weeks, 4 weeks, 6–8 weeks, 6 months and 1 year
Forest & Ray is a private dentist in London (Holborn, Camden) offering a wide range of treatments (basically everything), same-day appointments 7 days a week and affordable prices. The key behind a beautiful smile is self confidence, and success. At Forest & Ray we ensure to help you to the best of our ability. If you place your trust in us, we will make sure you achieve your goals and maintain oral hygiene to the maximum of its capacity. Regardless of any age or condition, we promise painless treatments and a professional team.